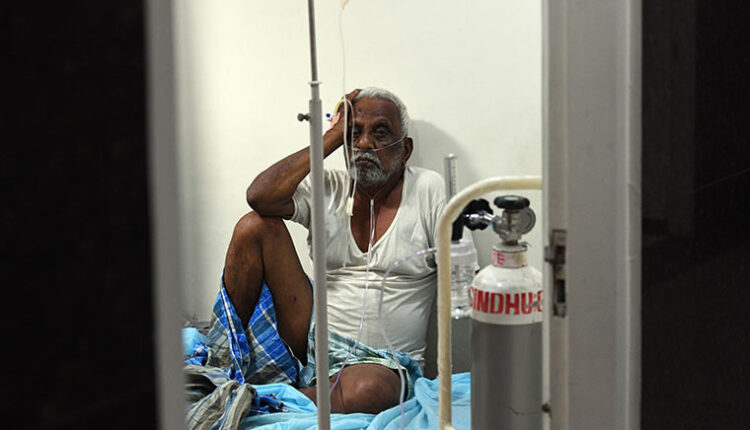
What caused India’s oxygen crisis amid COVID-19 pandemic
This story first appeared in The Week
When the tsunami hit India in 2004, the world offered to send relief material. India, however, politely refused the aid, saying it had the wherewithal to take care of its own. In the 15 years hence, India whittled down existing aid packages to almost a bare minimum. Instead, it positioned itself in the league of donors, increasing its development cooperation budget every year, rebuilding Afghanistan, taking care of the neighbourhood and reaching out to Africa.
India thought it was atmanirbhar, and had the basics of roti, kapda, makaan (food, clothing and shelter) almost sorted out; it had not imagined that it would have to go about asking for air to breathe. So, when a flight landed from the UK on April 27 with a donation of oxygen concentrators and ventilators, it gratefully accepted the charity. “Beg, borrow or steal [oxygen], it is a national emergency,” the Delhi High Court recently told the Centre, as blood-numbing tales of patients dying for want of oxygen began pouring in from everywhere. Senior ministers and bureaucrats then began making desperate calls overseas. Subsequently, apart from the UK, France, Germany, Australia and Ireland have announced their aid packages; Russia and Kuwait are likely to do so, too. Even Bhutan, forever the recipient, has assured 40 metric tonnes of liquid oxygen daily. The US has made grand announcements, but not quantified the assistance so far. US Inc, from Amazon to Microsoft, has enumerated the assistance it will extend.
Meanwhile, the Indian Air Force rushed to ferry emergency oxygen purchases from Singapore, Bangkok and Dubai, and to courier the gas from one part of the country to another. The Centre ordered a ban on industry use of oxygen, with exceptions like medical, pharmaceutical and defence.

For a nation, which till recently, was exporting oxygen, (in fact, its exports doubled over the last year), this clamber for oxygen, as well as essential medicines, is not only ironic, but also telling of the poor planning, internal squabbling and an institutional smugness over having supposedly suppressed the pandemic.
The second wave rose sharper than the first, yet, there was reaction time, if only the authorities had heeded. “The political class was busy with elections. The bureaucracy should have been alert; it is their job to prepare, plan and oversee crisis management,” said former home secretary G.K. Pillai. “They had time, at least a few months to fill the gaps, create infrastructure… but they took their eyes off the ball.”
The cost of this mismanagement is great in human life, but there is an economic loss, too. “Emergency purchases are at the price quoted. Are we importing at a price higher than we exported?” wondered Malancha Chakrabarty of Observer Research Foundation. “Would it not have been prudent to stock up, given that the pandemic has not receded from the world?”
A Union health ministry comparison of hospital admissions over the last year has shown that this time, there is a 13 per cent increase in oxygen beds. The analysis does not explain why this is so, neither does it factor in the increased oxygen demand for home patients. The ventilator demand, on the other hand, dropped by 10 per cent. Percentages, however, do not indicate the denominator, which is massive this time, and in sheer numbers, oxygen, ventilators and medicines supplies are being strained.
There are multiple reasons for the increased demand. The UK variant that is dominating the north spreads faster, and thereby, entire localities are falling ill, leading to a strain on local infrastructure, said epidemiologist Archisman Mohapatra, executive director, Generating Research Insights for Development (GRID) Council.
It has not helped that the infrastructure set up last time, instead of being augmented, had actually been dismantled. Bengaluru happily wrapped up the massive field hospital it had set up last year; today, its patients are scouring for beds in Mysuru, Hubli and nearby towns. In Delhi, while the Centre and state may blame each other for the situation, the truth is that neither stopped the other from pulling down jumbo facilities that the Defence and Research Development Organisation and Indo-Tibetan Border Police had put up; they had to be revived all over again. The Sardar Patel Covid Care Centre and Hospital in Chhatarpur admitted its first patient on April 26, much after the daily death toll had crossed the 300 mark. The ITBP facility had 123 admissions on the day of reopening.

But was it just shortage, or more of mismanagement, which caused patients to gasp to their deaths? In Delhi, Chief Minister Arvind Kejriwal complained of supplies being stopped at the borders, ultimately forcing the Centre to invoke the Disaster Management Act and allow free movement of the life-giving gas. However, within cities, there was initially no coordinated supply mechanism. “Instead of giving a decent reaction time of 12 hours, hospitals sometimes suddenly announce that they will run out of supply within a matter of hours,” said Sachindra Pratap Singh of Mumbai’s oxygen supply task force. Such panic cries from ministers and hospitals have resulted in a thriving black market for not just oxygen cylinders, but also vital medicines like remdesivir. According to industry sources, the existing oxygen production capacity in India, including in steel plants, is around 8,000MT a day. The Covid-19 surge has put the daily demand at around 6,500MT. It is the distribution, rather than production, which is the bigger problem, said Siddharth Jain, director of INOX Air. Most production is in east India, with some in Karnataka and west India, said Hanuman Mal Bengani, former CEO, Linde India. The demand, on the other hand, is in north India—Delhi, Punjab, Uttar Pradesh—as well as Maharashtra and Gujarat. At the beginning of the second surge, authorities were caught napping when the oxygen demand escalated. The Railways launched its Oxygen Express service on April 21, way after the wave had already caused enough devastation.
The blame game continues. According to the home ministry, Delhi government’s management was poor. Union home secretary Ajay Bhalla wrote to the Delhi chief secretary pointing out that the city did not arrange oxygen tankers in time, even though the Centre had made allotments. He said Delhi was allocated 480MT on April 21, after assessing the requirement, but it received less than the allocation because of logistical reasons not addressed by the state. Telangana has learnt from the experiences of Delhi and secured oxygen supplies from Odisha.
In Nashik, it was not a shortage of supply but a leak in the oxygen tank that caused the death of 24 patients on life support. The Centre’s core team on Covid management, including NITI Aayog member V.K. Paul and AIIMS chief R.K. Guleria, is now giving tips on how to prevent oxygen wastage, and for prudent use of this precious resource.
Meanwhile, even as India looked outside for air, the Sterlite plant at Thoothukudi, Tamil Nadu, a facility capable of producing 1,050MT oxygen daily, remained shut. Its owners appealed for the gates to be unlocked, but the state government did not agree for a precious long time. In court, advocate general Vijay Narayan said the plant could only produce 35MT of the required liquid oxygen. The plant finally has been given conditional permission to run for four months to produce oxygen.
The situation with the drug and vaccine shortage is even more embarrassing, given the positioning India did last year as the ‘pharmacy and vaccinator of the world’. Today, it is receiving drugs in aid. The Vaccine Maitri outreach has come to an embarrassing halt, with neither exports materialising, nor the supplies being adequate for the forthcoming programme of universal adult vaccination from May. The long lines are back—for oxygen cylinders, medicines and beds. “We are back to the India of the 1970s,” said Chakrabarty. “India lost much of its high ground with the migrant crisis last year. The oxygen crisis this year has dented our international image badly. We thought we had a seat at the high table and were part of the global decision-making process, here we have been exposed at not being able to handle our own mess.”
The coming days are likely to be worse, with the Empowered Group of Officers (EG-1) under Paul warning the Centre to prepare for a five to six lakh daily rise of cases by May before the curve dips. With the aid coming in, supplies may be secured for the present. But if there is any lesson that the second wave has taught, it is that the endgame is far away. “Typically, pandemics come in several surges, spread over a couple of years, before settling down as endemics,” said Mohapatra. A third wave is a distinct possibility, even a fourth. Will we be caught napping again?
With Namrata Biji Ahuja, Lakshmi Subramanian, Pooja Biraia Jaiswal, Abhinav Singh and Rahul Devulapalli
